Urinary strictures, a condition that can cause significant discomfort and a host of urinary problems, often go undiagnosed for too long. A urinary stricture is essentially a scar that narrows the urethra, the tube that carries urine from the bladder out of the body. When this tube becomes constricted, it makes it difficult for urine to flow freely. While the symptoms can be frustrating and even alarming, a proper diagnosis and treatment plan can bring immense relief and prevent further complications. This article will provide a comprehensive overview of urinary strictures, from what they are to the latest treatment options.
What Are Urinary Strictures?
A urinary stricture is the result of scar tissue forming within the urethra. The scar tissue causes the tube to become narrow, restricting the passage of urine. This can happen anywhere along the length of the urethra, but is most common in the part of the urethra that passes through the penis. The narrowing can be a small, isolated area or a longer segment. When the urine Urinary Strictures, flow is blocked, it can cause the bladder to work harder, and over time, this can lead to bladder, kidney, and prostate problems. It is a condition that is more common in men than in women due to the longer length of the male urethra.
Causes of Urinary Strictures
The formation of a urinary stricture is almost always linked to some form of injury or inflammation to the urethra. The body’s natural healing process creates scar tissue to repair the damage, but this can lead to the narrowing of the channel. The most common causes include:
Trauma or Injury: A direct injury to the groin or pelvis, such as a fall, a sports injury, or a pelvic fracture, can damage the urethra and lead to a stricture.
Infections: Sexually transmitted infections (STIs) like gonorrhea and chlamydia are major causes of urethral inflammation (urethritis) that can result in strictures.
Medical Procedures: Urethral instrumentation, such as catheterization, cystoscopy, or even some prostate treatments, can sometimes cause microscopic damage that leads to scar tissue formation.
Congenital Conditions: In rare cases, a person may be born with a stricture.
Lichen Sclerosus: This is a rare, chronic inflammatory skin condition that can affect the urethra and cause strictures.
Recognizing the Symptoms
The symptoms of a urinary stricture often develop slowly over time. They are primarily related to the obstruction of urine flow. If you experience any of these, it’s a good idea to seek medical advice:
Weak urinary stream: The most common symptom is a noticeable decrease in the force of your urine stream.
Spraying or splitting stream: The urine stream may not be a single, straight line.
Difficulty urinating: You may have to strain or push to start urination.
Incomplete emptying: The feeling that your bladder is still full after you’ve finished urinating.
Pain during urination (Dysuria): A burning or painful sensation when you urinate.
Urinary Tract Infections (UTIs): A blocked urethra can cause urine to sit in the bladder, increasing the risk of infection.
Blood in the urine (Hematuria): Though less common, blood may appear in your urine.
In severe cases, a stricture can lead to a complete inability to urinate, which is a medical emergency known as acute urinary retention.
Diagnosis and Evaluation
Diagnosing a urinary stricture requires a urologist’s expertise. The process typically begins with a thorough medical history and a physical exam. The doctor may also order several tests to confirm the diagnosis and determine the location, length, and severity of the stricture:
Uroflowmetry: This simple test measures the speed and strength of your urine flow. A weak flow can indicate an obstruction.
Retrograde Urethrogram (RUG): This is a key diagnostic tool. A special dye is injected into the tip of the penis, and X-rays are taken to visualize the entire urethra and pinpoint the exact location and length of the stricture.
Cystoscopy: A small, flexible scope is inserted into the urethra to allow the doctor to directly view the stricture and assess its characteristics.
Ultrasound: This may be used to look at the bladder and kidneys for signs of damage or to measure how much urine is left in the bladder after urination.
Treatment Options for Urinary Strictures
The goal of treatment for a urinary stricture is to open the urethra and restore normal urine flow. The best treatment option depends on the length and location of the stricture and the patient’s overall health.
Urethral Dilation: For short or less severe strictures, a doctor may pass progressively larger instruments into the urethra to stretch and widen the narrowed area. This is a temporary solution, and the stricture often recurs over time.
Internal Urethrotomy: In this procedure, a small scope is inserted into the urethra, and a tiny blade or laser is used to cut through the scar tissue. Like dilation, this can be effective for short strictures but has a high recurrence rate.
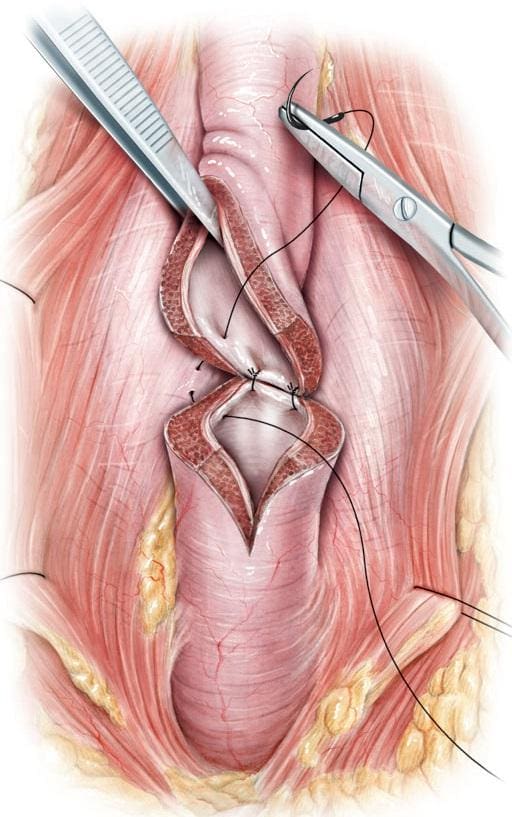
Urethroplasty: This is considered the gold standard for long-term correction of urethral strictures. It is a reconstructive surgical procedure that involves removing the scarred section of the urethra and rejoining the healthy ends. For longer strictures, a graft from the patient’s cheek, tongue, or foreskin may be used to rebuild the urethra. While more invasive, urethroplasty has a very high success rate and is a durable solution.
Permanent Stent Placement: In some cases, a permanent stent may be placed to hold the urethra open, although this is a less common option.
The decision on which treatment to pursue is a serious one, and it’s essential to have an open conversation with a urology specialist who can explain the pros and cons of each option.
FAQs About Urinary Strictures
Q: Can a urinary stricture heal on its own?
A: No, once scar tissue has formed, a urinary stricture will not heal on its own. It requires medical intervention to be treated.
Q: Is urethroplasty a major surgery?
A: Urethroplasty is a significant surgical procedure, but it is highly effective. It is often performed as an outpatient procedure or with a short hospital stay, and recovery can take several weeks.
Q: What is the risk of a stricture recurring after treatment?
A: The risk of recurrence varies greatly by treatment type. Urethral dilation and urethrotomy have high recurrence rates, while urethroplasty has a very high success rate, often exceeding 90%.
Q: Can women get urinary strictures?
A: Yes, although it is much less common due to the shorter length of the female urethra. When they do occur, it is often due to trauma or repeated catheterization.
Q: Will a stricture affect my sexual function?
A: A stricture itself does not directly cause erectile dysfunction. However, the anxiety associated with the condition or some of the treatments may temporarily impact sexual function.
Choosing Expert Care
Living with the symptoms of a urinary stricture can be a source of constant frustration and worry. A weakened stream, the need to strain, and the fear of a urinary blockage can disrupt your life. The good news is that with the right diagnosis and treatment, you can find a lasting solution. For expert care and a compassionate team dedicated to your urological health, the specialists at Urology Partners Of North Texas are here to provide the guidance and treatment you need.